Look Back in Wonder
A father searches for the secret to empathy in the face of unthinkable loss
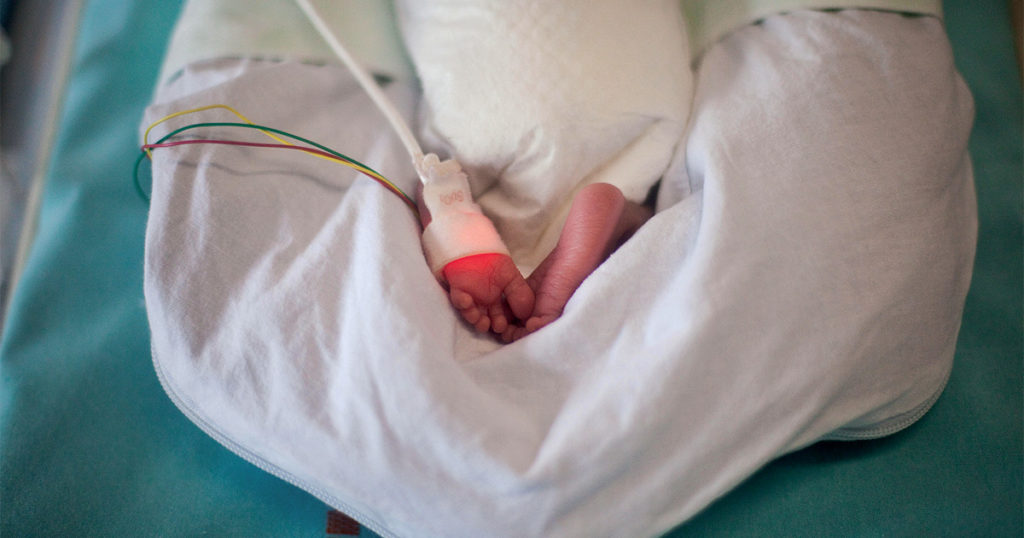
On a wet, gray afternoon in February 2007, the rain turning to snow as the light faded and the temperature dropped, my wife delivered our second child: a boy, like our first, and, like our first, a surprise. We’d learned of the pregnancy only a few weeks before we moved to Appleton, Wisconsin, where I was to begin teaching at a small liberal arts college. It had been a taxing fall and winter: Wisconsin was darker and colder than any place my wife or I had ever lived, we knew no one in our town, and early ultrasounds of the fetus had shown signs of a lethal genetic anomaly, requiring a series of expensive and invasive tests. The results, thankfully, had come back negative, but on New Year’s Eve, my wife started bleeding, and we rushed to the hospital, fearing premature labor. The obstetrician scheduled an induction for a week before our son’s due date. Despite the difficult road we’d traveled, the doctor assured us, the baby was healthy, and everything would be fine.
When the nurse handed him to us, wrapped in a blanket, rosy and warm, he did seem fine. But when she opened the blanket on the warming table to measure his temperature, weight, and length, she saw that his chest had turned gray, his lips a dull lavender. His five-minute Apgar score, which assesses vital signs, was lower than his one-minute. His skin was pale; his arms and legs had gone floppy, unresponsive to stimulus; and his breathing was shallow. My mother-in-law, a veteran pediatric nurse in a major children’s hospital, stood over her grandson with her lips pursed. She cooed gently to him and reassured the delivery nurses that they were doing a good job, but her face gave away her concern.
Chest x-rays revealed fluid in his lungs. Later tests would warn of an enlarged heart. The snow was falling harder, sticking to the windows and whiting out the cars in the parking lot. The labor and delivery nurses were growing anxious. My wife, who had worked as a medical social worker in the same children’s hospital as her mother, recognized the nurses’ anxiety for what it meant: the baby was too sick to stay in the regional hospital. That evening, a specialized nurse in a blue jumpsuit threaded an intubation tube between our son’s vocal cords, connected his lungs to a ventilator, and handed him off to two mustachioed paramedics, who loaded him into a portable incubator and wheeled him through the empty hospital corridors to an ambulance waiting outside. They drove him a half-hour south to a hospital with a NICU—a neonatal intensive care unit. My wife and I followed behind. The windshield wipers struggled to stay ahead of the blizzarding snow, and I lost sight of the ambulance halfway through what felt like an interminable journey. I drove in silence while my wife, one day postpartum, cradled her stomach and tried not to cry. I’d never been so scared in my life.
After 10 days, our son’s lungs had recovered enough for him to come home. The heart issue, too, had resolved as his lungs responded to the medication. The day of his discharge, the neonatologist posed for a picture with him before the nurses helped us secure his carrier into the back seat of our car. I was sure I’d feel calmer once we got him home—I’d been fantasizing about his homecoming since the night of his birth.
Instead, I had trouble sleeping. I lay in the dark and listened to his faint exhalations, worried that he would spontaneously stop breathing. As the days moved forward and winter melted into spring, the minute-by-minute ticktock playing in my mind of my son’s birth, decline, and hurried admission to the NICU began to collapse into a nebulous dread, one that subsumed even the initial happy memories of his arrival. I felt as if I were watching a city recede in my rearview mirror, all the buildings and parks and freeways merging into a hazy skyline in which the NICU remained the only recognizable structure.
In a stroke of either dumb luck or divine providence, two weeks after our son’s discharge from the hospital, my wife accepted a position as a social worker at the NICU in St. Elizabeth Hospital in Appleton—a different hospital from the one where our son was treated, though it was similar in size, capacity, and level of care, and it served the same northeastern Wisconsin community. This meant that my wife essentially returned each day to the site of what had been our worst nightmare: the same assembly of ventilators, incubators, monitors, IV pumps, and bilirubin lights that had surrounded our infant son. The prospect of working in such an environment terrified me, but my wife welcomed it. She felt she better understood the agonized worry of the parents in the NICU now that she had endured the same worry herself, and she felt a special bond with the fragile newborns, some weighing barely more than a pound.
It was my wife’s responsibility as the unit’s sole social worker to ensure that babies would be discharged to safe home environments. She screened parents for postpartum depression and housing insecurity and helped them apply for Medicaid. Most of the babies in her unit—a Level III NICU—survived, which meant that their parents’ experiences largely echoed ours: a frightful beginning gradually giving way to a return to normal life. The most acute cases, those requiring surgical interventions, were transferred to Level IV NICUs in Madison or Milwaukee. Rarely, though, a baby would be born too early or too sick to save. On those nights—and the worst tragedies often seemed to occur in the dead of night—my wife would go the distance with the families, talking the parents through the decision to withdraw treatment, then staying in the room while they held their children for the first and final time. Each evening, when she arrived home from work, I plied her with questions. I wanted to know everything she’d seen, everything that had happened. I could envision these stories so clearly, as though they were happening not to strangers but to me.
In June, we attended the wedding of one of my wife’s coworkers, a neonatologist. After the ceremony, we accompanied other members of the NICU staff to a local brewpub. I happened to sit beside a nurse who had recently started working in the NICU at the Minnesota children’s hospital where a young couple had given birth a few weeks earlier to sextuplets. They’d been conceived with the help of the fertility drug Follistim, which had caused the mother’s ovaries to release multiple eggs in one ovulation cycle. The couple’s doctors had urged them to “reduce” the number of fetuses, but the parents, both deeply religious, had refused.
The sextuplets were born at 20 weeks of gestation, a full month shy of their third trimester and only halfway to full term. The heaviest of the six weighed a whopping 19 ounces, the smallest only 11. They were among the smallest human beings ever to be born alive, and by the time I sat beside the nurse that day, three of the babies had died. Two more would perish by the end of July, leaving only one survivor: a boy. The birth of the sextuplets, followed by the seemingly endless cascade of losses, had made national news. I watched the reports obsessively, recalling my own terrified days and nights in the NICU when I stood over my son, watching his chest retract and counting his breaths. Some in the media had likened the parents to fanatical crackpots who’d landed in a mess of their own making. But I couldn’t do that, not after what my wife and I had been through. That would have felt like a denial, or worse, a betrayal.
The thought of witnessing my son’s death, which had once seemed so near, could still make me cry. The idea of watching five children perish one by one was too much to comprehend. When I asked the nurse what it had been like, being in the NICU with the family, her eyes welled up. Along with the parents and the other members of the staff, she’d had no choice but to stare down into death’s abyss and fathom its depth. Our own abyss had been shallower, and we’d forestalled going over the edge—my son was now four months old, smiling and lifting his head when laid on his belly—but still, I felt I could relate. I’d yet to entertain the possibility of one day writing about the NICU, but at the brewpub that afternoon, I felt I needed to listen, to bear witness to the things the nurse had seen.
The nurse seemed eager to talk, as though she’d been waiting for someone to ask her about the sextuplets. I leaned on my elbow, nursed my beer, and hung on her every word.
My wife had worked in the NICU for five years by the time I started working on a novel set in the unit. We’d attended holiday parties, retirement sendoffs, bowling nights, and summer cookouts, and several members of the staff—including the doctor whose wedding we’d attended—had become close friends. In all that time, I’d never stopped thinking about the family of the sextuplets. They’d started a website at the time of the pregnancy and occasionally posted updates. The baby who’d survived was nearly the same age as my own son. He had some mild cerebral palsy and retinopathy, both resulting from his extreme prematurity, but he seemed pretty healthy otherwise. In photographs, he could be seen playing and smiling beside his parents and two younger sisters. I couldn’t say whether they were happy, but they seemed to have charted a path forward. “People think that being in here is the end of the world,” a NICU nurse had told me as we’d stood together beside my son’s bed. “They don’t understand that there’s a place in the world for sick babies.”
The novel I’d begun borrowed a page from the sextuplets’ story, though the mother in my story becomes pregnant with four babies instead of six. Given the option to reduce the pregnancies, she demurs, and when she goes into labor after just 23 weeks, she and her husband find themselves plunged into the NICU’s arcane world of flashing alarms and hissing ventilators, roller-coastering through hope and loss until they can hardly tell one from the other. The parents’ story entwines a second narrative, of a long-time nurse struggling to care for her troubled teenage son, himself a former preemie. I wanted to take my characters—whom I imagined as fiercely loving and spurred by good intentions—past their breaking points, not to wallow in their misery but to see if I could bring them to a place of redemption. I also felt an obligation to testify, in the most honest terms possible, to the whipsawing intensities of the NICU, the messy lives of the medical staff, and the anguish of the mothers and fathers holding vigil beside their imperiled children.
To aid in my writing process, I compiled a reading list of every NICU-related book I could find. There weren’t many: a smattering of memoirs published over the course of two decades and practically no novels. Desperate to learn more, I contacted the volunteer coordinator at my wife’s hospital and offered to do any task, no matter how menial, so long as it was in the unit. I took a brief orientation class, pledged not to release any medical information relating to the babies or their parents, and was given a name badge and a blue vest to wear over my shirt.
For six months, I folded laundry, restocked supply carts, and answered phones. I sanitized equipment and got reacquainted with the noises and smells of the unit, albeit this time without the panic brought on by every blinking light and honking sound. Some weeks, there would be a frenetic rush of admissions, the doctors working around the clock for several days in a row, and a week or two later, the unit would empty and the staff would spend the morning gossiping at the nurse’s station. During the slower spells, I reorganized the medical supply closet and assembled brochures into admission packets, which my wife would give to incoming families.
When things really slowed down, I’d duck into a corner and scribble in my notebook.
I watched so many parents—from partnered couples to single moms, Volvo-driving yuppies to teenagers from impoverished farming towns—fidget beside their infants’ beds, feverishly bouncing their knees while they stared at the clock on the wall. Other parents tried to pretend that nothing out of the ordinary had occurred, perhaps hoping that if they acted normally and practiced some magical thinking, they could will a happy outcome into existence. I started to see the NICU as occupying a kind of vortex within the larger hospital. The unit was adjacent to labor and delivery, the one hospital wing where people routinely went not in sickness but in health, expecting only good things to happen: that babies would tumble into the world, healthy and vernix-coated, attended by video cameras and balloons. The NICU, in contrast, lay behind a nondescript locked door that most visitors, patients, and even hospital employees breezed by, without bothering—or daring—to look inside. To have a baby rushed from the delivery room to such a place was to be yanked rudely away from the happy fantasy, like a fish plucked from a stream.
When I talked about the novel, even in broad terms, people often winced. Babies in peril—babies dying—were the stuff of tasteless jokes and sentimental charity commercials. More than one person told me that the book sounded, in a word, dark. Once, over dinner, a fellow writer and English professor began to cry after hearing about my research. When I told my agent I’d found very few books, and hardly any novels, set in the NICU, a fact I believed would be a mark in my favor, she replied, “Well, there could be a reason for that. Bleak stories are hard to sell.”
For the record, I’m not by nature a dark person. I can’t handle violent thrillers, slasher flicks, or zombie movies, nor am I drawn to such commercialized literary genres as “misery lit” or “trauma porn,” which aim to titillate readers through gratuitous depictions of suffering and pain—and risk dehumanizing and exploiting the very people they depict. I envisioned my novel to be something deeper: not trauma porn, not just a sad story, but a tragedy.
Aristotle’s definition of a tragedy—“an imitation of an action that is serious, complete, and of a certain magnitude”—says as much about the genre’s formal specifications as its content. A tragedy must be organized around a reversal of fortune ( peripeteia in Greek) in which a persecuted hero is restored to nobility. Or, more commonly, the protagonist is brought low by his flawed choices and the stirrings of fate and chance. Although tragedies don’t have to end with the entire House of Denmark lying dead on the floor of Elsinore, pain and agony still reside at the core of the genre. It’s by witnessing the suffering of another human being (and we shouldn’t forget that for most of history, tragedies have been performed live and in person) that an audience moves toward anagnorisis, recognition, and from there to catharsis, the “purgation of pity and fear.”
Because pity and fear frequently travel together, they can be mistaken for synonyms. In truth, however, the emotions oppose each other. Fear is an emotion of inferiority: the perception that someone, be it a human or a god, can harm us and those we love. Pity stems from the belief that another’s suffering is somehow beneath us; we’re superior to them. Fear aggrandizes our enemies; pity aggrandizes us. It’s hard to pity those we fear, and hard to fear the pitiful, though that’s exactly tragedy’s aim: to elicit both emotions simultaneously and in equal amounts. Audience members are forced to see themselves reflected in the characters’ self-destructive mistakes. “Ah, that is he,” Aristotle writes, by which he means, He is me. Tragedies leave us drained, purged—catharized, Aristotle would say—but also humbled and a little wiser, at once tougher and a little softer, a little less gullible and a little more human. “You emerge from tragedy equipped against lies,” writes Howard Barker in Arguments for a Theatre. “After the musical, you’re anybody’s fool.”
Even more than fostering resilience, tragedy generates sympathy—a quality I find in short supply during these troubled, divisive times. Pop intellectuals such as Brené Brown have rendered sympathy the ugly stepsister of empathy: Brown describes empathy as “feeling with” and denigrates sympathy as “put[ting] a silver lining” around another’s pain. The Greek roots of “sympathy,” however, sym and pathos, more accurately denote “feeling with,” whereas empathy connotes an excess of emotion projected toward another (and in modern Greek, empátheia even means malice or malevolence). Empathy, moreover, did not enter the English language until the 20th century, whereas sympathy is far older, used by both David Hume and Adam Smith to describe the process by which a person may vicariously experience the emotions of another. In recent years, sympathy has also come to mean something like concern for the people with whom we already identify, reserved for the righteous and denied to the sinful. Yet according to George Eliot, sympathy requires the recognition of one’s personal limitations and the effort to reach beyond those limits—a “deeply-awing sense of responsibility to man,” she writes. The characters in her novels who stand the best chance of escaping isolation are those who, like Silas Marner, develop a “consciousness of dependence” on others. Rebecca Solnit echoes this sentiment precisely in A Paradise Built in Hell: The Extraordinary Communities That Arise in Disaster:
A friend tells me, as I write, of someone we know who has joined a support group for his grim disease; these groups create communities of sufferers so that one feels neither alone nor marked out uniquely for suffering. The religious contemplation of suffering and work with the sick, the poor, and the dying likewise serve to develop compassion and subvert tendencies to self-pity and its twin, self-aggrandizement.
Unlike trauma porn, then, which invites gawking from a safe distance, tragedy asks us to see life close up. If trauma porn dehumanizes its subject, tragedy rehumanizes. Tragedy joins us together. It reminds us that we are our brothers’ keepers after all.
I came to understand this on a more personal level when, around the same time I began working on the NICU novel, I also started writing short, humorous essays about my sons, who were then seven and five and locked in an utterly toxic and codependent relationship—they fought like dogs yet couldn’t stand to be apart from each other. These essays were only a few pages long and usually centered on a single moment of awkwardness, like the time I tried to explain the history of Saint Nicholas to my older son, who promptly marched into his kindergarten class and announced that the real Santa Claus was dead. Or the time I threatened to wash out my younger son’s mouth with soap if he continued to swear at school and, in an ill-conceived attempt to demonstrate the punishment, ended up washing out my own mouth. Whenever I’d finish an essay, I’d read it to my family and friends, sometimes to an entire party of guests, and they’d howl with laughter. I’d never thought of myself as particularly funny, at least not on the page, and it felt good to hear people laugh.
Yet it was the harder stuff, my closely guarded experiences of pain and indignity, that resided closer to my heart. These formed the stories I told my closest friends, the ones who’d stick around the party after the other guests had left, who’d help with the dishes and trash and then follow me to the couch, where, in the orange glow of firelight, we’d enter the hour when tragedies were told. Revealing my dark secrets and listening while my friends offered up their own injuries and mistakes, I could feel us drawing closer together. For all their discomforts and agonies, their purgations of pity and fear, tragedies are ultimately love stories.
Back in 2012, I’d been volunteering in the NICU for a few weeks when a baby was admitted to the unit. He’d been born at 21 weeks of gestation, even though his mother had been on bed rest in the hospital for close to a month. His trachea was so small that the doctors had a hard time intubating him and, at one point, paused to ask the mother if she wanted them to keep trying. He was the smallest, sickest baby in the unit, which also made him the smallest, sickest baby in the hospital, my city, and that entire corner of Wisconsin. On several occasions, the chief neonatologist urgently summoned the parents to the hospital because their son was on the verge of dying. The parents’ relationship frayed; even at the baby’s bedside, the tension was palpable. The nurses seemed invested in the marital drama until they weren’t. When the baby was transferred to the children’s hospital in Madison for surgery, the entire staff felt relieved.
Three years later, I tracked the mother down and asked if she’d meet me for coffee. I was at a low point in my writing; after years of research and drafting, I’d gotten lost in the weeds, and every time I sat down to work on the book, I felt a certain dread, doubting my motivations for writing it in the first place. Even if I managed to finish the damn thing, I wondered, who would ever want to read about such sorrows?
The mother and I arranged to meet at our local Starbucks on the Friday before Thanksgiving. The place was decked out with glittery snowflakes and miniature evergreen trees adorned with lights and ornaments. Her son came with her; he was three years old but looked closer to two: a wobbly toddler with a moon-size noggin. He had a horizontal scar in his neck from a tracheostomy that had once connected his lungs to a ventilator. He’d been dependent on the machine the first two years of his life. “When we left the NICU in Appleton, I was told to expect he’d be on a vent for the rest of his life,” his mom said to me. “The pulmonologist in Madison promised me he’d be breathing on his own by kindergarten. And look! He’s only three.”
“Impressive.”
“So many people told me to let him go,” she said. “Especially in the beginning. He’s my little fighter.”
As we sipped our lattes, she filled me in on her son’s progress. After leaving Appleton, he’d had nearly a dozen surgeries and spent many months in and out of the hospital, first in the NICU and then, once he’d passed a year, the pediatric ICU. He still needed a lot of therapy, and her insurance didn’t cover much of it. She and her son’s dad hadn’t been together for a while now. She tended bar at night while her son stayed with her parents. One day, she said, she’d like to go back to nursing school, but she was living paycheck to paycheck these days.
I said that must be hard. She shrugged, then nodded.
Her son sat on her lap with a book he didn’t seem much interested in. He squeaked and gurgled but didn’t say anything I could identify as an actual word. I offered to buy him a muffin, thinking that something bready and sweet might occupy his attention, but his mother declined. His years on the ventilator had disabled his ability to swallow and to talk, and though he could breathe without the help of a machine, he had to eat through a gastronomy tube in his abdomen. At three, he knew enough about food to know it went in the mouth, but even a small bite could become lodged in his throat and cause him to choke.
The Starbucks grew crowded, and the little guy became overstimulated. He began to squirm on his mom’s lap and cry. I could tell she was growing flustered, and I offered to call it a day, but she suggested we finish the conversation over tea, at her parents’ house nearby.
Once there, she carried her son inside and laid him in his bed. He’d required round-the-clock nursing care when he’d first come home from the hospital, so she and her son had lived with her parents for a while. They still kept a room for him with a crib and rocking chair, as well as a green oxygen canister the medical supply company had never bothered to collect once he’d come off the ventilator; it stood in the corner as a testament to how far he’d come in his short life. After peeking inside his room, I waited for her in the kitchen while she got him settled.
We sat across from each other at the round wooden table. I had my notebook open, though I hadn’t written very much. Steam curled up from our mugs of tea. The house was quiet. “What else do you want to know?” she asked.
I thought for a moment. “I want to know what it’s been like for you. All of this.” I gestured at the kitchen, though she knew what I meant. “You have a good attitude, but I’m sure it’s been rough.”
She leaned back in her chair and crossed her arms. She stared at me for a long moment, as if measuring whether she could trust me. I wanted to look away, but I did not dare. Then, to my surprise, her eyes filled. She dabbed at the tears with the back of her hand. “No one knows,” she said. “No one knows what it’s like. How hard it is. Even my parents don’t totally get it. No one does.”
She looked at me as if maybe I got it. I hoped that after everything I’d seen, all the effort I’d put in, I did get it. She cried a little harder. She didn’t resent her son, she said, or regret the decisions she’d made to save his life. Nor did she regret her tumultuous relationship with her son’s dad, despite how things turned out. She only wished that the people in her life had a better sense of what it was like to hold a child so close to the edge of life and to wonder, each day, whether he would stay or go—and whether, in light of his pain, her grief, and the doctors’ confusing and discouraging advice, she was selfish to fight so hard to keep him. “I want to read your book when you’re done,” she said.
“Of course,” I said. “If I ever finish it.”
“You will. You have to.”
“I’ll keep at it.”
“You’d better,” she said. “I’ll be disappointed if you don’t.”
I said goodbye and got back in my car. I had an appointment in Green Bay, so I headed north. Past the edge of our small city, the farmlands opened up. Plowed fields stretched all the way to the horizon. The November sky was heavy and gray-brown, the color of tea with too much milk, though in spots the sun broke through, spotlighting the tarry roofs and rolled hay bales. I watched the clouds turn orange and pink and made a promise that no matter what, I’d keep trying till I got the story right.


