Of Plagues and Prejudice
Whether cholera or Covid-19, epidemic disease can reveal what is hidden—in ourselves and our societies
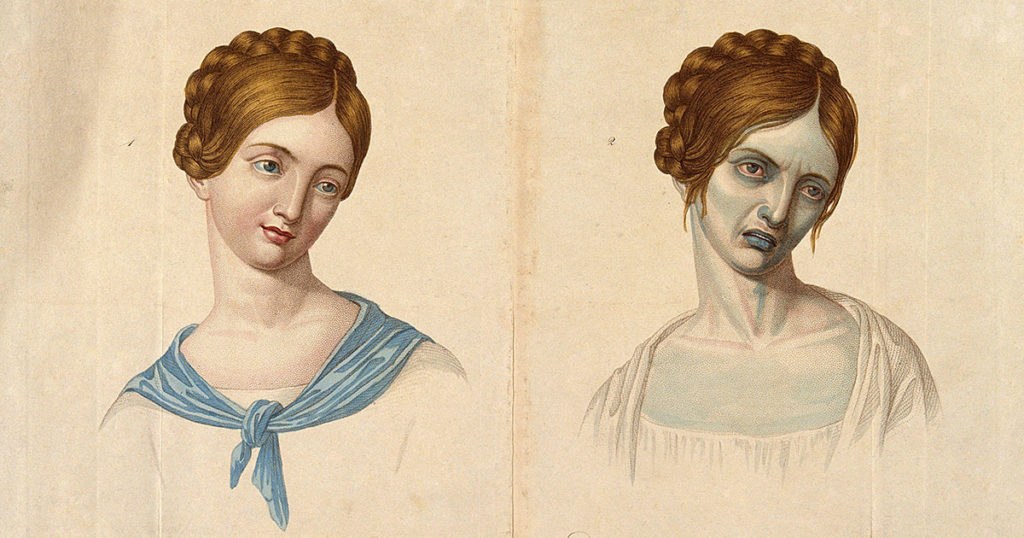
Pandemics make us think about the plagues of the past. As we live through the time of Covid-19, we seek lessons from other moments when microorganisms caused widespread death and devastation. In the 19th century, cholera put great cities into states of fear and flight and left whole families lying dead, even as physicians debated causation and transmission, and governments wrestled with travel regulations, immigration restrictions, and mandatory quarantines.
There is a cholera vaccine now, though its efficacy is not perfect or long lasting, and the disease can be treated, but epidemic cholera remains a problem in regions blighted by poverty, war, or natural disaster. Cholera continues to kill, especially where medical resources and access to clean drinking water are limited. In 2010, a severe outbreak started in Haiti that eventually killed nearly 10,000 people. But as a pediatrician treating children in the United States, I have never seen a case of cholera.
I am interested in diseases that, though no longer a threat to my patients, have shaped human history, leaving traces of their malignant presences in memory and in literature. And at this pandemic moment, we need to remember what we have learned from past pandemics: that humans everywhere, in the 21st century as in the 19th, are more closely connected than they sometimes want to believe, and that microorganisms accompany us when we travel, thrive when we gather together, and exploit our inequalities. Cholera offers us a history of scientific and epidemiologic detection, but also a history of scientific and epidemiologic error. It reminds us of the successes and the failures of quarantines and border restrictions, and it cautions us to consider most carefully how we live with the waste that we produce.
On June 26, 1832, the first case of cholera in New York City broke out among members of an Irish immigrant family, the Fitzgeralds. The father was the first to get sick; he recovered, but both of his children and their mother died. The United States and Canada had been watching nervously for cholera, relying on the Atlantic Ocean to keep them safe from an epidemic raging in Europe.
Earlier in the century, cholera had emerged as an epidemic disease in Asia. No one knew the cause, but we now understand that the bacteria that cause cholera live in copepods—tiny plankton that exist in brackish water—and spilled over into humans in the Sundarbans, the mangrove swamps of Bengal. In Pandemic (2016), science journalist Sonia Shah describes how, in 1817, deforestation and agricultural practices under the auspices of the British East India Company generated a major cholera epidemic. The British blamed it not on their own colonial undertaking but on a range of Indian religious practices and lapses in hygiene. Thousands of people died in Asia, but Europeans regarded the epidemic as remote. However, by 1830, cholera had spread from Asia, across Russia, the Middle East, and into Western Europe, traveling with armies, with sick passengers aboard ships, and in the water that steamships used for ballast.
In France, 100,000 people died, and despite British quarantine efforts, the disease killed thousands in London in 1832. On June 6, 1832, cholera appeared in Montreal and began moving south. New York City worriedly awaited its first cases, just as in early 2020 the city braced for the arrival of Covid-19. In The Cholera Years (1962), medical historian Charles Rosenberg describes how people of means prepared to flee eastern cities for their country homes while groups of doctors set out for Montreal and Quebec to study the disease. Meanwhile, the New York City Board of Health set up quarantine policies to keep ships out, appointed health officers to disinfect the streets with chloride of lime, and required doctors to report any cases they saw.
By June, cholera had arrived in the United States, and from its original points of entry in Whitehall and other upstate New York canal towns, it traveled across the country by river and canal, by road and railroad. Mortality was high in New York City that summer, but it was also bad in New Orleans and Chicago. John Pintard, the well-to-do banker who founded the New-York Historical Society, stuck out the summer in the city, confident that he had nothing to fear from a disease “almost exclusively confined to the lower classes of intemperate dissolute & filthy people huddled together like swine in their polluted habitations.” Clergy pointed to the deaths of prostitutes and drunkards to suggest that the virtuous were safe. The death rate was high among new immigrants, especially the Irish crowded together into city slums, and African Americans. Enslaved people in the South suffered disproportionately, but so did impoverished free Blacks living in the North: in Philadelphia, they died at twice the rate of whites.
Many of the old cities of Europe had outgrown their historical sanitary arrangements. London had two million people and could no longer rely on its system of outhouses, cesspools, and waste collectors. In the United States, new “frontier” cities like Cincinnati had no infrastructure to safeguard their rapidly growing populations. The combination of human crowding and poor sanitation was what made these cities particularly vulnerable to cholera, which spreads when infected human waste contaminates drinking water or food. But in the 1830s, none of this was clear; many doctors, in fact, were “anti-contagionists,” believing that cholera was an “atmospheric” disease rather than something that spread from person to person. They viewed quarantine as an old-fashioned and unscientific approach, contending that people who got sick were vulnerable because of their own bad habits. Quarantines, of course, were also deeply disruptive to trade, which made them politically unpopular. Having traced the progress of cholera along the canal system from Canada to New York City, Dr. Lewis Beck, in a report to the governor, insisted—against his own carefully gathered evidence—that the disease was not actually contagious, since it affected only “persons of irregular habits,” people who ate bad diets, or drank too much, or lived in the wrong part of town.
Epidemics recurred across the United States in 1849, and again in 1866. In 1849, more than 5,000 people died in New York City, but in 1866, the Metropolitan Board of Health organized quarantine and disinfection efforts and helped the city escape the worst. Chicago, which had been hit harder, soon established its own board of health. “Cholera in 1866 was a social problem; in 1832, it had still been, to many Americans, a primarily moral dilemma,” Rosenberg writes. Rosenberg, now an emeritus professor at Harvard, told me that the reform efforts in the United States from the 1830s to the 1880s reflected both a growing awareness of the risks built into urban crowding and changes in scientific understanding of disease. “Rationalizing water supply, cleaning the streets, milk and food inspection—in retrospect they look perfectly rational,” he said, but the interplay of science and politics was “complicated, subtle, not always apparent.” Americans continued to respond to cholera with days of prayer (President Zachary Taylor proclaimed a national fast in 1849), and moralistic—and sometimes xenophobic—lessons about hygiene and bad habits continued to be drawn. But increasingly, in the second half of the 19th century, the fear of cholera and the growing understanding that it was connected in some way to dirt and human waste drove the creation of public health infrastructure, especially in cities.
Cholera remained a worry into the 20th century, with a serious outbreak in India beginning in 1899 and spreading to Eastern Europe. In the United States, as the new century approached, cholera fueled growing nativist hostility against immigrants arriving from Europe. In Quarantine! (1997), physician and medical historian Howard Markel writes of the ways in which anxiety about cholera came to be focused on immigrants from Eastern Europe, many having embarked for the United States from Hamburg, where a major epidemic was raging. In 1892, when cholera broke out among both steerage and cabin-class passengers aboard the Normannia, a quarantine was imposed. From his first-class stateroom, E. L. Godkin, the founding editor of The Nation, mocked the public-health doctor for his apparent unawareness that cholera “is exceeding rare among the well-clothed, well-fed and cleanly class in any country.” To a certain extent, he was right: the death rate was far higher among passengers on the lower decks, where sanitary conditions were poor.
The experience of passengers aboard the Normannia and other ships, forced to quarantine offshore, brings to mind the many cruise-ship travelers who faced an eerily similar stasis during the early days of the Covid-19 pandemic. Cholera is a profoundly different disease from Covid-19, yet its depiction in the literature of its time—often lurking ominously at the edge of the page—carries new resonance.
All epidemic diseases have their own pathological personalities, and for the most part, when they show up in the arts, there’s a certain medical realism that excites the interest of doctors reading for identifiable signs and symptoms. The Decameron opens with a description of buboes, “the appearance of certain swellings in the groin or the armpit, some of which were egg-shaped whilst others were roughly the size of the common apple.” Tuberculosis, with its ethereal wasting pallor, is a famous presence in literature and music; the wracking cough it causes is a part of the plot of Verdi’s La Traviata (1853) and Puccini’s La bohème (1896), as well as Eugene O’Neill’s 1956 play Long Day’s Journey Into Night, in which Edmund Tyrone’s every suspicious cough reminds you that he’s bound for the sanitarium. In Pierre Choderlos de Laclos’s Liaisons dangereuses (1782) and Charles Dickens’s Bleak House (1853), smallpox leaves those it fails to kill disfigured or blind.
Cholera, however, is different. It casts a literary shadow of contagion and gloom, as befits what Rosenberg calls “the classic epidemic disease of the nineteenth century, as plague had been of the fourteenth.” But even so, when cholera turns up in literature, its identifiable hallmarks are usually invisible, presumably because the mechanisms by which it wipes out its victims were too unpleasant to contemplate.
In The Secret Garden, Frances Hodgson Burnett’s much-beloved 1911 novel about children and the healing powers of nature, cholera breaks out “in its most fatal form” among the servants of the British Lennox family in India. Nine-year-old Mary Lennox finds herself alone in a lavish bungalow. Her parents and many of the servants are dead, so she is sent to live with an uncle she has never met in his remote mansion in Yorkshire, where the moors and the gardens will work their magic on her. In the novel, cholera appears matter-of-factly as an unsurprising piece of the medical history of Anglo-Indian relations. Burnett depicts the disease as swift and terrible (and most definitely from Asia) but suggests nothing of its effects on the human body: the severe watery diarrhea, combined with vomiting, during which victims rapidly lose fluids and electrolytes. It should not surprise us, then, that no 19th-century opera heroine dies, on stage, of cholera.
Dickens began his last completed novel, Our Mutual Friend (1865), with an account of scavengers along the River Thames who discover a corpse floating in the muck. But Dickens, despite being aware of the filthy water that flowed through London, may not have connected it specifically to disease and did not invoke cholera in his fiction. Instead, it turns up in his journalism and his social activism: he wrote a series of four impassioned articles in 1849 after 180 children died of cholera at the Juvenile Pauper Asylum at Tooting, eight miles outside London. The institution was run by Bartholomew Drouet, and the children were undernourished, crowded together, and poorly cared for. The establishment, Dickens wrote, was “brutally conducted, vilely kept, preposterously inspected, dishonestly defended, a disgrace to a Christian community, and a stain upon a civilized land.” Drouet was brought up on murder charges, though he was acquitted, since it could not be definitively proved that the cholera was his fault.
Five years later, in 1854, Dickens’s oldest daughter, Mary, came down with cholera while the family was traveling in France. “She was sinking so fast,” Dickens wrote to novelist Wilkie Collins, “and the sickness was so exceedingly alarming. … Thank God, she recovered so favourably that by breakfast time she was fast asleep.” Cholera, in the middle of the 19th century, was a cause for social reform when it devastated a “pauper farm,” but it was also something that could strike a member of a prosperous author’s family, on a comfortable trip of fine hotels, theatrical performances, and lavish dinners.
People get infected with cholera by ingesting Vibrio cholerae bacteria, generally in water that has been contaminated with sewage or in food that has been contaminated with that water. Many of the infected display no symptoms, but in those who get sick, a toxin affects cell membranes causing sodium, potassium, and especially chloride to leak into the intestine, sucking the water out of cells and into the gut, leading to watery diarrhea full of infectious bacteria. Victims can lose as much as a quart of fluid per hour. Losing 10 percent of your body weight this way means severe dehydration; losing 15 percent can be enough to kill you, especially with the accompanying electrolyte losses. In severe cases, death comes in a matter of hours. “Cholera beds” or “cholera cots” used in outbreaks have holes cut in the center so that the diarrhea can be collected in a bucket below.
The methods by which many European and American port cities attempted to keep out cholera dated back to outbreaks of bubonic plague in the 14th century. Quarantines had first been imposed in 1377, in Dubrovnik, where travelers were required to spend a month on an isolated island before entering the city. But the word quarantine was coined only later, in Venice—a reference to the 40-day period that ships had to sit at anchor before passengers and crew disembarked. Venice also built the first dedicated plague hospital, or lazaretto, in 1423, and soon other port cities followed suit, setting up remote facilities to tend to the sick. The name lazaretto made hopeful reference to the resurrection of Lazarus, but the trip to a plague hospital was often a trip of no return. At the time, there were no effective treatments for bubonic plague, just as half a millennium later, there was nothing doctors could do for victims of cholera.
Instead, physicians observed the agonies of their patients in minute detail. One British physician wrote of “great debility, extinction of the circulation, and sudden cooling of the body … accompanied by exhausting evacuations of a peculiar character, intense thirst, cold blue clammy skin, suffused filmy half-closed eyes, cramps of the limbs, extending to the muscles of respiration.” Left unaffected was the victim’s intellect: people dying of cholera were perfectly aware of what was happening to them.
Each step in the process of infection and bodily destruction took time to decipher. In London in 1854, Dr. John Snow tracked those who had sickened and died in a cholera outbreak, street by street, house by house, and ultimately pump by pump. He concluded that the unifying factor in exposure to cholera was that victims had drunk water from the Broad Street pump. He could not point to bacteria, which were not yet well understood, but he used his map to argue against the prevailing “miasmic” theory of disease, which held that breathing foul air caused the infection.
In 1846, Dr. Edwin Chadwick, author of the influential 1842 British Poor Law Commissioners’ Report on the Sanitary Conditions of the Labouring Population of Great Britain, had told a parliamentary committee that “all smell is disease.” To reduce the odors emanating from cesspools in crowded neighborhoods, the city had responded by diverting sewage into the Thames, likely putting more Londoners at risk when the disease came back. Snow’s great epidemiologic achievement—his “death map” of an outbreak in Soho, which attempted to show that people with cholera were sick not from noxious vapors but from drinking water—did not meet with general acceptance for several decades.
Presciently, Snow insisted that the handle be removed from the Broad Street pump to prevent it from dispensing its lethal water. The epidemic was probably already subsiding, but his action made a historic (and correct) point about waterborne transmission and the need to protect the water supply from contamination. More than 10,000 people died of cholera in that London epidemic in the mid-1850s, but not until the Great Stink of 1858, four years after Snow shut off the Broad Street pump, did members of Parliament, their workplace made untenable by the stench from the Thames, pass the legislation to create London’s sewer system. They thought the danger was in the smell of the polluted river, not in the microbes it carried.
Snow knew there was something in the water but couldn’t say what it was. The bacterial cause had actually been identified as early as 1854 (the same year Snow disabled the pump) by Italian anatomy professor Filippo Pacini, who found a comma-shaped organism in the intestinal mucosa of people who had died in a cholera epidemic in Florence. He published his finding, but the sentiment in Italy strongly favored the miasma theory, and few took note of this alternative explanation. In 1884, the cholera bacterium was discovered all over again, this time by German physician Robert Koch, one of the founding fathers of bacteriology, who also identified the bacterial cause of tuberculosis. Koch called the organism that he believed caused cholera Der Kommabazillus, though many scientists still remained unconvinced by his discovery. Scientists did, over time, come to understand that bacteria did the damage, not foul smells. Still, the role of the cholera toxin that poisons the intestinal cells was not understood until 1959, when Sambhu Nath De, a professor at Calcutta Medical College, identified the toxin and showed that even when all the bacteria were filtered out, it could still cause the disease. And new discoveries are still being made: as recently as 2018, researchers at Harvard Medical School found that a bacteriophage—a virus that infects the cholera bacteria—carries the gene sequence that encodes the toxin. Only Vibrio cholerae bacteria infected with this filamentous, or hairlike, viral particle, produce the toxin.
In 1849, Harriet Beecher Stowe and her husband, Calvin, were living in Cincinnati, where Calvin was a professor of theology. The town was a busy center for commerce, riverboat traffic, and the hog trade. Known as “Porkopolis,” it was teeming with pigs, which helped clean the streets by eating from piles of heaped-up garbage. When a cholera epidemic erupted that summer, Calvin was taking a “water cure” in Brattleboro, Vermont. In a letter dated June 29, Harriet warned him not to return to Cincinnati, lest he get sick. “To exchange the salubrious air of Brattleboro for the pestilent atmosphere of this place,” she wrote, “with your system rendered sensitive by water-cure treatment would be extremely dangerous.” She continued to write to him, chronicling the spread of the plague. “Gentlemen make themselves agreeable to ladies by reciting the number of deaths in this house or that,” she wrote on Independence Day. “This together with talk of funerals, cholera medicines, cholera dietetics, and chloride of lime form the ordinary staple of conversation.”
Harriet was caring for their six children, who ranged in age from 13-year-old twins, Hattie and Eliza, to one-year-old Charley. As young as Charley was, he had been weaned by the time cholera arrived and was therefore vulnerable to waterborne infection. On July 10, Harriet wrote to Calvin, “Yesterday little Charley was taken ill, not seriously, and at any other season I should not be alarmed. Now, however, a slight illness seems like a death sentence, and I will not dissemble that I feel from the outset very little hope. I still think it best that you should not return.” However, despite her initial sense of despair, there was more promising news to report two days later: “He is evidently getting better, and is auspiciously cross. … Anna and I have said to each other exultingly a score of times, ‘How cross the little fellow is! How he does scold!’ ” And on July 15: “Charley apparently recovering, but still weak and feeble, unable to walk or play, and so miserably fretful and unhappy.”
By July 23, though, the boy’s condition had deteriorated again: “We have been watching all day by the dying bed of little Charley, who is gradually sinking. … About four days ago he was taken with decided cholera, and now there is no hope of his surviving this night.” Three days later: “My Charley—my beautiful, loving, gladsome baby, so loving, so sweet, so full of life and hope and strength—now lies shrouded, pale and cold, in the room below. … I have just seen him in his death agony, looked on his imploring face when I could not help nor soothe nor do one thing, not one, to mitigate his cruel suffering, do nothing but pray in my anguish that he might die soon.”
Calvin assured his grieving wife that Charley was only gone to heaven a little before the rest of them, and he wrote to all the other children to say that little Charley never had the chance to sin—and demanded of them sternly, could that be said of them? But Harriet Beecher Stowe, in the novel that would make her famous and change the world, drew a different set of morals from Charley’s death: in the grief and anguish that she had felt at Charley’s grave, she had come to understand, she said, “what a poor slave mother may feel when her child is torn away from her.” Charley could not be saved, but those other separations could be prevented by ending the evil trade of slavery. “No one knows fully what it is to live till they have stood helpless by, to see the death struggle of what was dearest to them,” Harriet wrote to a friend. There was nothing to be done about cholera, but grieving mothers could help put an end to a different horror:
By the sick hour of your child; by those dying eyes, which you can never forget; by those last cries, that wrung your heart when you could neither help nor save; by the desolation of that empty cradle, that silent nursery—I beseech you, pity those mothers that are constantly made childless by the American slave-trade!
Uncle Tom’s Cabin was serialized in 1851–52 in The National Era and went on to become the best-selling novel of the century.
Cholera epidemics continued to rage into the 20th century, just as the disease continued to play a role in literature. Writers still avoided visceral descriptions of diarrhea or vomiting, lest they offend their readers’ sensibilities. Instead, they often invoked cholera to suggest an overpowering sense of dread and death.
This is the case with Thomas Mann’s 1912 novella, Death in Venice. The protagonist, Gustav von Aschenbach, has been wandering through Venice in pursuit of a young Polish boy, Tadzio, with whom he is obsessed, and has become aware of ominous intimations—people speaking of a plague, the disinfectant scent of carbolic. Finally, an honest young Englishman at a British travel bureau names the peril: “Asiatic cholera” from “the hot, moist swamps of the delta of the Ganges, where it bred in the mephitic air of that primeval island-jungle.” It has spread across Afghanistan, Persia, and Russia and has now attacked several ports on the Mediterranean. The Venetian authorities are trying to keep things quiet, insisting publicly that Venice is healthy, but food is already contaminated, and the infection is spreading in the canals. “Eighty out of every hundred died, and horribly, for the onslaught was … of the ‘dry’ type, the most malignant form of the contagion,” Mann writes. “In this form the victim’s body loses power to expel the water secreted by the blood vessels, it shrivels up, he passes with hoarse cries from convulsion to convulsion, his blood grows thick like pitch, and he suffocates in a few hours.” The travel agent advises Aschenbach to leave Venice immediately, but he cannot bring himself to leave Tadzio. Then, very gently, Aschenbach sickens, experiencing “spells of giddiness only half physical in their nature, accompanied by a swiftly mounting dread, a sense of futility and hopelessness.” He dies quietly, sitting in his beach chair.
“If mentioned at all, cholera has been understood as a symbol or as a motif variously interpreted in psychoanalytical, sexual-pathological, political or mythological terms,” writes Thomas Rütten, a historian of medicine who has traced Mann’s own experience with the Venetian cholera epidemic of 1911. For Rütten, “one of the last European cholera epidemics, after all a major event, forms one of the novella’s central themes.” Mann and his wife were on vacation in 1911, traveling to the Adriatic island of Brioni, now part of Croatia, and then to Venice on May 24. The city authorities had attempted to keep cholera out of Venice, and now that it had arrived, they were engaged in a cover-up, keeping any mention of the epidemic out of the press, under the direction of the national government. According to Rütten, one reason for the official silence was that a large celebration was planned for June 4 in Rome, to mark the 50th anniversary of Italian unification and to unveil the enormous monument to King Vittorio Emanuele II that still stands in the center of the city.
Even if the Italian press was silent, the German-language newspapers were not. Mann, like his character Aschenbach, encountered much talk of cholera when he got to Venice. Yet unlike Aschenbach, the Manns cut their trip short and left the city, indeed aided by a helpful clerk at the Thomas Cook travel agency. “Reviewed with the benefit of hindsight and from a medico-historical perspective,” Rütten writes, “Thomas Mann’s account of cholera in Venice is characterised by a rare and almost preternatural insightfulness into an otherwise murky affair that was marked by rumours, speculations, and dementi. The city (and its authorities) is diagnosed by the writer with unfailing accuracy.” The last outbreaks of cholera in Europe coincided with the early decades of mass Mediterranean tourism, creating awkward intersections and sometimes a culture of dishonest denial.
A decade later, William Somerset Maugham found in cholera the threat and menace he needed for his novel The Painted Veil, in which a British doctor punishes his unfaithful wife by taking her into a zone of contagion, hoping she will get sick and die. Thus the Chinese town of Mei-tan-fu, site of the worst cholera epidemic in years, becomes the backdrop for infidelity and a marriage coming apart. Maugham’s couple, Kitty and Walter Fane, have access to a cholera “inoculation”—from a vaccine developed in 1885 that was the first to defend against bacterial disease in humans, although it offered only imperfect protection. They have also been advised by a local British official on how to stay safe: “Have your milk and water boiled and don’t eat fresh fruit or uncooked vegetables.” As part of their twisted game of marital chess, however, Kitty makes a point of eating salad. When Walter warns, “You’ll kill yourself,” she responds, “I thought that was the idea.” From then on, the two of them eat salad together every night. For all this, though, the only time we see a specific symptom of cholera is when Kitty is suddenly taken ill: “nausea overwhelmed her and she vomited.” Kitty assumes that her vomiting marks the onset of cholera, but the drama turns out to be more domestic in nature: she is pregnant, without knowing whether the child belongs to her husband or her lover. When Walter is stricken (from having contracted cholera in the course of his bacteriological investigations, and perhaps from having deliberately experimented on himself), he looks too sick to live. But Maugham does not describe specific symptoms—and even has Walter shed tears (however unlikely, given the extreme dehydration cholera brings) as Kitty begs for forgiveness.
If you search for literary references to cholera, you inevitably come upon Gabriel García Márquez’s 1985 novel, Love in the Time of Cholera, a title that resonates in headlines about our current pandemic. (Google the phrase “love in the time of Covid” and you’ll get 3.36 billion results.) García Márquez offers the story of two elderly, lifelong lovers, Fermina Daza and Florentino Ariza, who look back to cholera as a disease of the past; the “time of cholera” was when they were young and first fell in love. Florentino, as a young man, had been stricken with gastrointestinal symptoms, just when he had fallen madly in love with Fermina:
He lost his voice and his appetite and spent the entire night tossing and turning in his bed. … His anguish was complicated by diarrhea and green vomit, he became disoriented and suffered from sudden fainting spells, and his mother was terrified because his condition did not resemble the turmoil of love so much as the devastation of cholera.
The mother consults a homeopathic practitioner, who is alarmed at how the young man looks: “he had the weak pulse, the hoarse breathing, and the pale perspiration of a dying man. … All that was needed was shrewd questioning, first of the patient and then of his mother, to conclude once again that the symptoms of love were the same as those of cholera.”
Epidemic diseases often reveal what is hidden—in our bodies, in our private lives, in our societies. Cholera forced us to rethink how we dispose of human waste. By the middle of the 20th century, the disease had been “solved” not by medicine but by sanitation. But in the 19th century, cities and nations faced deadly waves of the illness without a clear understanding of how it spread. They tried quarantines and travel restrictions, which we continue to employ in our own pandemic moment. Like Covid-19, cholera generated xenophobia, quack medicine, and cover-ups. It pitted public health imperatives against the exigencies of international travel and commerce. And as with Covid-19, discovering cholera’s microbial cause—and the mode of its transmission—helped to halt the spread of the disease without necessarily providing therapies that would save the lives of those people already stricken. The mainstay of medical therapy for cholera, the essential idea that was missing in the 19th century, is rehydration, with either oral fluid or, in severe cases, intravenous solution. The bacterial infection can also be fought with antibiotics, but to keep the patient alive, the clinical imperative is to prevent the toxin from doing its work, to give fluid and electrolytes to avoid that abrupt and fatal drying-out and shutting-down of the body.
Like other pandemic stories, cholera reminds us of how the stresses and threats of deadly epidemic disease emphasize and exaggerate the fault lines in our societies—what Rosenberg calls a “stress test.” Covid-19 has vividly illuminated our own social fault lines, the inequalities of health and risk built into every aspect of how we live, work, and travel. Pandemics invariably raise the question of what groups are most at risk, just as they remind us, whatever our prejudices and politics, that because we all have bodies, we are all vulnerable.


